Mortality Rates Between Black and White Americans Explained
admin April 2, 2025Science News ArticleMortality rates Black and white Americans reveal a troubling narrative about healthcare disparities that persist in the United States. Despite significant advancements in medical technology and healthcare access, the gap in mortality rates between these two racial groups persists, particularly among infants. A recent study highlighted that while both Black and white Americans have seen improvements in life expectancy, Black infants face disproportionate risks, dying at rates significantly higher than their white counterparts. This stark reality emphasizes the urgent need for effective public health policy to address these racial health inequalities in America. As we delve into the factors contributing to these disparities, it’s crucial to consider the broader implications of our healthcare system on the well-being of the nation’s most vulnerable populations.
The discussion surrounding the disparities in death rates between Black and white Americans is critical to understanding broader social and health issues. Racial health inequalities in the U.S. highlight systemic flaws within healthcare delivery, often resulting in poorer outcomes for minority populations. While life expectancy figures offer a glimpse of progress, they overshadow the alarming segment of infant mortality rates, where Black infants are disproportionately affected. As we examine the factors behind these alarming statistics, it becomes clear that addressing disparities is not just a matter of improvement in healthcare access but also about ensuring the quality of care received by all racial groups. It is essential for policymakers to prioritize comprehensive strategies that mitigate these long-standing inequalities.
Understanding Mortality Rates among Black and White Americans
Recent research has highlighted the narrowing gap in overall mortality rates between Black and white Americans over the decades. In the 1950s, life expectancy was significantly lower for Black Americans, but improvements over the ensuing years have resulted in an increase in life expectancy to 76 years. In contrast, white Americans have also seen life expectancy increase to 79.3 years. Despite these advancements, significant disparities in mortality rates persist, particularly among infants, where the situation is markedly dire with Black infants facing a mortality rate that is twice as high as their white counterparts.
The implications of these findings are profound, indicating an urgent need for targeted public health policies to address these ongoing disparities. While life expectancy has improved for both groups, it is crucial to recognize that this does not present a complete picture of health equity. Healthcare disparities, especially in infant mortality, suggest that systemic issues in healthcare accessibility and quality still exist. This signals that enhancement efforts should focus comprehensively on reducing these inequalities, rather than concentrating solely on broad health improvements.
The Widening Gap in Infant Mortality Rates
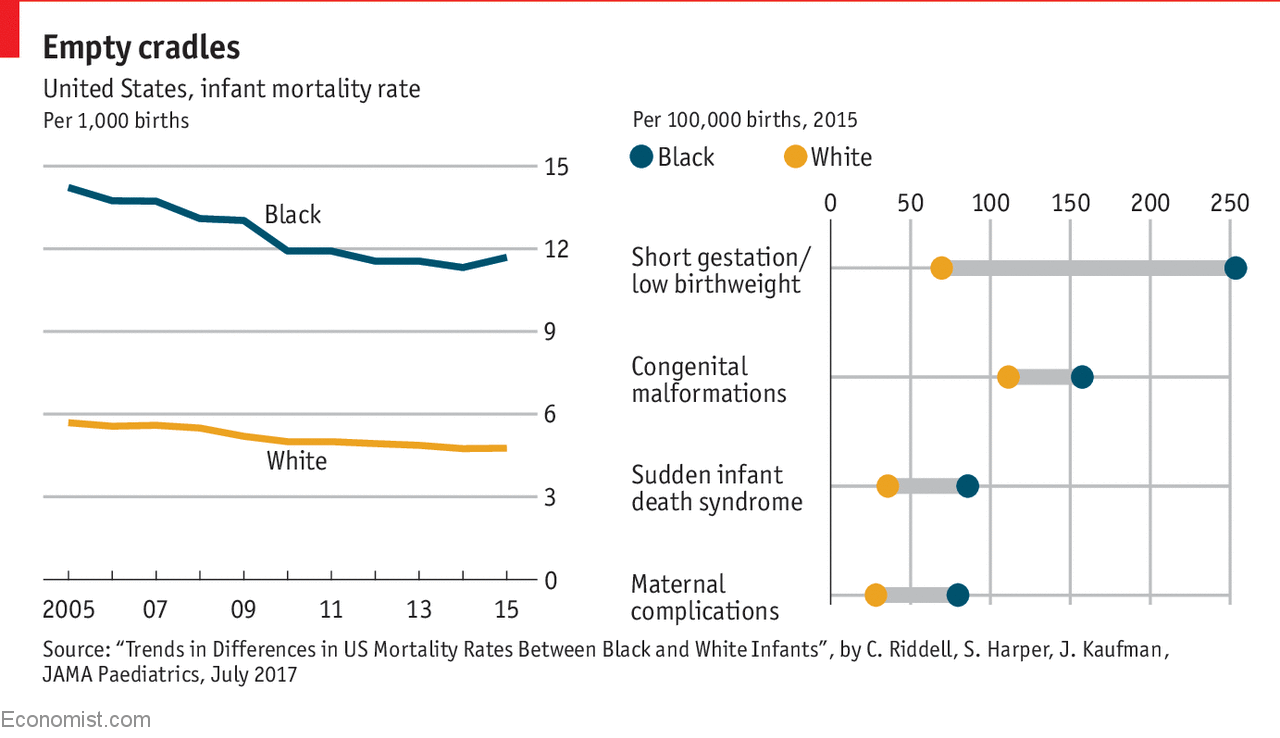
Infant mortality rates provide a stark indicator of healthcare disparities between racial groups. As findings indicate, while mortality rates have improved for both Black and white infants, the gap has actually widened, with Black infants experiencing a shocking 115% higher mortality rate than white infants today. This is a troubling statistic that requires immediate attention, particularly because infant mortality is often linked to healthcare access and quality during prenatal and postpartum care.
This uptick in disparity reflects systemic health inequities that have persisted over decades and signals that improvements in healthcare, though evident, have failed to equally benefit all populations. Notably, the leading causes of death for Black infants can often be attributed to medical conditions related to pregnancy. This highlights a critical area for public health interventions focusing on maternal health and equitable healthcare access that ensures both quality and availability of services, which are essential in curbing such alarming rates.
Public Health Policy and Racial Health Inequalities
As research indicates, the findings of narrowed mortality rates overall juxtaposed with widening gaps among infants create a paradox that public health policies must address. The historical context shows that while life expectancy has seen improvements, health disparities particularly in vulnerable populations remain stubbornly persistent. Public health policy traditionally focused on improving broad health metrics, yet this approach has not been effective in narrowing racial health inequities.
Moving forward, policymakers must prioritize strategies that specifically target the underlying causes of these disparities. This includes ensuring access to quality prenatal care for Black mothers, addressing the socio-economic factors contributing to health disparities, and fostering community-based health initiatives. By implementing targeted public health policies, it is possible to make strides toward achieving equitable health outcomes for all racial groups in America.
Life Expectancy Improvements: A Double-Edged Sword for Racial Groups
The recent analysis of life expectancy improvements shows remarkable progress over the last 70 years for both Black and white Americans. For Black Americans, life expectancy increased from 60.5 years to 76 years, while white Americans improved from 69 to 79.3 years. This data reveals an overall trend towards increased longevity; however, it also highlights a complex narrative where broad improvements in life expectancy mask the persistent disparities that exist, particularly in infant mortality rates.
These improvements should not overshadow the reality that significant gaps remain between racial groups. While both categories have benefitted from advancements in healthcare, the disparities experienced in their respective health outcomes necessitate a focused approach. Policymakers need to analyze these statistics critically and develop interventions tailored not just to improve healthcare metrics on a general scale, but specifically to lift the most vulnerable populations.
The Role of Healthcare Disparities in Black Infant Mortality
Healthcare disparities play a crucial role in understanding the higher mortality rates for Black infants compared to their white counterparts. Factors such as access to prenatal care, quality of healthcare facilities, and the socio-economic status of families contribute significantly to this issue. The data illustrates that, even with a general progression in healthcare standards, Black infants continue to be at a disadvantage, directly affecting their chances of survival.
Addressing these disparities requires a multifaceted approach involving healthcare providers, policymakers, and community organizations. Fostering initiatives that ensure equal access to quality healthcare, particularly for pregnant women and infants, can be instrumental in reversing these alarming trends. Furthermore, continuous evaluation and adjustment of health policies that aim to reduce racial health inequalities will be essential to establish a more equitable health landscape.
The Impact of Historical Context on Current Mortality Rates
Understanding the historical context of healthcare disparities provides insight into today’s mortality rates among Black and white Americans. For decades, systemic racism and discrimination in healthcare systems have created barriers that have disproportionately affected Black populations. Historical inequities have led to foundational differences in access to quality care, knowledge of healthcare resources, and representation within health policy frameworks.
Public health authorities must actively confront this historical backdrop to address the root causes of current disparities. Research findings call for urgent action, highlighting how the legacy of past injustices continues to affect health outcomes today. By implementing policies that recognize and address these historical factors, we can create a more just and effective healthcare system that prioritizes health equity.
Addressing Infant Mortality Through Targeted Interventions
With the stark contrast in infant mortality rates between Black and white infants underscored in recent studies, it is imperative that targeted interventions are developed and implemented. Recognizing the specific medical challenges faced by Black infants is the first step towards addressing this urgent public health crisis. Interventions that focus on improving maternal health and ensuring access to quality prenatal care can significantly impact the outcomes for Black infants.
Furthermore, public health practitioners must consider a holistic approach that takes into account the social determinants of health affecting families. Programs that provide support for expectant mothers, improve educational materials regarding infant care, and facilitate access to healthcare resources will play a pivotal role in reversing the trend of higher mortality rates among Black infants. Only through targeted action can we hope to bridge the gap in infant mortality and establish a path toward equitable health for all.
Future Directions in Research and Public Health Policy
Given the disparities highlighted in the recent study, future research must focus on deeper investigations into the underlying causes of the differential mortality rates. Understanding the specific medical, economic, and social factors that contribute to these inequalities is crucial for crafting effective policies that aim to improve health outcomes. Comprehensive research focused on comparative studies will also help in understanding how public health initiatives have historically succeeded or failed in addressing these disparities.
As researchers continue to uncover the complexities of healthcare disparities, it is vital that public health policymakers leverage these findings to inform strategic action. The call to prioritize funding and resources for communities disproportionately affected by high mortality rates cannot be overstated. By directing attention and resources wisely, we can aspire to improve life expectancy and reduce disparities among all Americans, particularly the most vulnerable.
The Need for a Holistic Approach to Healthcare
Addressing healthcare disparities requires a comprehensive and holistic approach that encompasses not just access but also the quality of care provided to marginalized communities. Initiatives must extend beyond immediate medical interventions to include broader social support systems that enhance the overall health of families. Effective public health policy should integrate educational, economic, and environmental factors that contribute to health disparities.
Fostering community engagement and participation in health policy development is also key to understanding the unique needs of different populations. By actively involving those affected by health disparities in the decision-making process, policymakers can ensure that the solutions implemented are practical, equitable, and ultimately effective in improving outcomes across all racial groups.
Frequently Asked Questions
What are the current mortality rates for Black and white Americans?
As of recent studies, the mortality rates indicate that Black Americans have an 18% higher mortality rate compared to white Americans. However, both racial groups have seen improvements in life expectancy over the decades, with Black Americans increasing from 60.5 years in the 1950s to 76 years in the 2010s.
How do infant mortality rates compare between Black and white Americans?
The disparity in infant mortality rates is significant, with Black infants dying at approximately twice the rate of white infants. Recent reports show that this gap has widened, with Black infant mortality rates being 115% higher than those of their white counterparts.
What factors contribute to healthcare disparities in mortality rates between Black and white Americans?
Healthcare disparities are influenced by multiple factors, including access to care, quality of healthcare services, socioeconomic status, and systemic inequalities. These factors contribute to the higher mortality rates observed in Black Americans compared to white Americans.
How has public health policy addressed mortality rates among Black and white Americans?
While life expectancy has improved for both groups, public health policy must prioritize reducing the existing healthcare disparities, particularly among infant mortality rates. Current policies need to focus on equitable healthcare access and quality to address the disparities highlighted in recent studies.
What historical trends have influenced mortality rates between Black and white Americans?
Historical trends show that while overall mortality rates have narrowed over the last 70 years, the gap in infant mortality has unfortunately widened. This suggests that systemic health inequalities have persisted, especially affecting Black infants.
What implications do current mortality rates have for future public health initiatives?
Current mortality rates highlight the urgent need for public health initiatives that specifically target and reduce racial health inequalities. Addressing the root causes of these disparities could potentially save millions of lives, particularly among Black Americans.
Why is it important to analyze long-term mortality rates between Black and white Americans?
Analyzing long-term mortality rates provides a comprehensive view of healthcare inequalities over time. It reveals persistent gaps that shorter studies may overlook, emphasizing the need for targeted policies to improve health outcomes for marginalized populations.
What role does life expectancy play in understanding mortality rates for Black and white Americans?
Life expectancy serves as a key indicator of overall health in a population. While improvements in life expectancy are noted for both Black and white Americans, understanding the nuances behind mortality rates reveals ongoing disparities that must be addressed.
How can research into mortality rates influence public health policy?
Research into mortality rates can inform policymakers about critical health disparities that require intervention. By highlighting excessive mortality among Black Americans, it encourages the allocation of resources and the formulation of strategies aimed at achieving health equity.
What are some potential solutions to reduce mortality disparities between Black and white Americans?
Potential solutions include increasing access to quality healthcare, addressing socioeconomic factors, investing in community health initiatives, and implementing policies aimed at reducing systemic inequalities within the healthcare system.
| Key Findings | Black Americans | White Americans | |
|---|---|---|---|
| Improvement in life expectancy since the 1950s | 76 years (from 60.5 years) | 79.3 years (from 69 years) | |
| Higher overall mortality rate compared to whites | 18% higher | N/A | |
| Black infants dying at twice the rate of white infants | 116% disparity | N/A | |
| Mortality rate for Black infants worsened since the 1950s | 115% higher | N/A | |
| Call for prioritization of healthcare equality | Needed | N/A | |
Summary
Mortality rates between Black and white Americans have shown some improvements over the last 70 years; however, significant disparities remain, particularly in infant mortality. Research indicates that while life expectancy has increased for both groups, the mortality rate for Black infants has nearly doubled in comparison to white infants. This alarming trend highlights the urgent need for targeted public health initiatives to address healthcare inequality and enhance outcomes for Black Americans. Policymakers must prioritize effective measures to bridge these gaps in healthcare access and quality to reduce mortality rates among disadvantaged groups.
You may also like
Archives
Calendar
| M | T | W | T | F | S | S |
|---|---|---|---|---|---|---|
| 1 | 2 | 3 | ||||
| 4 | 5 | 6 | 7 | 8 | 9 | 10 |
| 11 | 12 | 13 | 14 | 15 | 16 | 17 |
| 18 | 19 | 20 | 21 | 22 | 23 | 24 |
| 25 | 26 | 27 | 28 | 29 | 30 | 31 |